A Mannitol-Based Perfusate for Reversible 5-Hour Asanguineous Ultraprofound Hypothermia in Canines
by Jerry D. Leaf, Michael G. Darwin, and Hugh Hixon
Cryovita Laboratories, Inc.
10743 Civic Center Drive
Rancho Cucamonga, CA 91730
Previously unpublished paper
This work was carried on from 1984 thru 1987
ABSTRACT
The purpose of this study was to test the hypothesis that a mannitol-based, potassium-enriched perfusate similar in concept to standard organ preservation solutions would be effective for prolonged whole body asanguineous hypothermia. Dogs were placed on femoral-femoral bypass and supported with cardiopulmonary bypass during cooling to a rectal temperature of 10-12°C. The animals were then exsanguinated by perfusion with 4 L of a solution containing 210 mM mannitol and 35 mM KCl in place of NaCl as cooling continued to a rectal temperature of 4-5°C. Perfusion continued for at least 4 hours at or below 9°C and for 2 hrs. at or below 5°C. During warming, the asanguineous perfusate was replaced with blood and hemodialysis was instituted to normalize serum electrolytes. All dogs survived without long-term sequelae. These results confirm the feasibility of applying the lessons learned from clinical organ preservation research to the problems of systemic hypothermia and support and extend recent reports of canine survival following hypothermia with lactobionate-based perfusates.
Introduction
Hypothermia has provided extended periods of circulatory arrest for open-heart surgery (7, 21), aortic aneurysm repair (10), resection of renal cell carcinomas (19), and neurosurgical procedures (5). However, the complexity of these procedures has been sharply limited by the relatively brief period during which circulatory arrest can be tolerated at 18°C. Clinical attempts to cool to lower temperatures to attain longer periods of safe circulatory arrest have been precluded by unacceptably high rates of respiratory, neurological, and hematological complications (1, 6, 17). Recent experiments strongly suggest that these difficulties stem from the same factors that limited clinical organ preservation prior to the development of solutions that precluded cell swelling during cold exposure. In particular, a lactobionate-based perfusate has been shown to permit 2 hours of safe whole-body asanguineous hypothermia below 10°C, or one hour of cardiac arrest plus one hour of low-flow asanguineous perfusion (26, 27). Lactobionate, however, is required for 24-48 hour organ preservation, not for 2-6 hour preservation. We felt that for the periods that are clinically pertinent for hypothermic surgery and related applications, a much simpler and considerably less expensive perfusate based on mannitol would be equally effective. The results reported here confirm this prediction and demonstrate for the first time that systemic hypothermia can be maintained for periods as long as 5 hours with consistently satisfactory recovery after warming.
Materials and Methods
asanguineous perfusate
The composition of the perfusate used for total body washout is given in Table 1 [PDF file]. Six liters of perfusate were prepared the night before each experiment and stored on ice.
Preoperative
All animals received humane care in compliance with the Principles of Laboratory Animal Care formulated by the National Society for Medical Research and the Guide for the Care and use of Laboratory Animals prepared by the National Institutes of Health (NIH Publication No. 80-23, revised 1978).
Six mongrel dogs of both sexes, weighing from 22 to 27 kg, were fasted for 12 hours before the induction of anesthesia, but were allowed water ad lib. The animals were premedicated with 50 mg of chlorpromazine administered intramuscularly, and were anesthetized with 30 mg/kg of sodium pentobarbital (Nembutal) administered intravenously through an 18 ga Angiocath placed in the medial foreleg vein. The animals were intubated with cuffed endotracheal tubes and ventilated with a Harvard dual-phase control ventilator using room air. A rate of 12-18 respirations per minute, with an inspiration to expiration ratio of 1:3 and a tidal volume of 18 ml/kg, was used during initial induction of hypothermia; respiratory rate and tidal volume were subsequently adjusted to maintain paO2 and paCO2 in the desired ranges during cooling and rewarming. During asanguineous perfusion, the animals were ventilated with intermittent deep sighs using a bag-valve device to prevent atelectasis.
Hypothermia was initiated by surface cooling. The dogs were placed on a cooling blanket connected to a Blanketrol heater/cooler set to 0°C and covered with Ziploc bags of crushed ice. Both esophageal and rectal temperatures were measured to the nearest 0.1°C with a YSI Model 46TUC temperature meter. Heart rate and ECG were monitored using three limb leads on an Electrodyne Model CB121B recording system.
Sodium bicarbonate was infused as needed in combination with induced respiratory alkalosis to control pH according to the alpha-stat pH strategy (38). Respiratory alkalosis was induced by increasing the oxygen flow to the oxygenator to produce an average perfusate arterial pCO2 of 24 ± 7.9 (SD) mm Hg during deep hypothermic TBW.
The following agents were administered at the beginning of surface cooling. Atropine, 0.4 mg, was given to reduce mucus secretion. To avoid injury to the gastric mucosa during profound hypothermia, cimetidine, 4 mg/kg, was given to inhibit gastric HCl production, and Maalox, 50 ml, was given via gastric tube to neutralize acidic stomach contents (34). Metubine iodide, 0.2 mg/kg, was given to inhibit shivering during the induction of hypothermia, thus conserving skeletal muscle energy reserves and avoiding unnecessary heat production. Verapamil, 0.15 mg/kg, was given to help control calcium influx that may occur as a consequence of metabolic inhibition by profound hypothermia. Solumedrol, 30 mg/kg, was given as a membrane stabilizer. Mannitol, 2 g/kg, was given to help protect the central nervous system (CNS) against edema.
Cannulation
During surface cooling, the femoral areas were shaved and prepped with Betadine solution and sterile drapes were applied for initiation of sterile technique. Both femoral veins and arteries were exposed in preparation for cannulation, with electrocautery for hemostasis. The right and left femoral arteries and veins were ligated distally with #1 silk. Heparin, 420 mg/kg, was administered intravenously before cannulation. A stainless steel perfusion cannula was placed in the right femoral artery through an arteriotomy made with a #11 scalpel blade and secured with a #1 silk tie. Venous return cannulae, USCI Type 1967, size 20 or 22 French, were introduced through venotomies in the right and left femoral veins and secured with #1 silk ties. Central venous pressure (CVP) was monitored by an Intracath, 17 ga x 24″, introduced through the right venous cannula via a side port in the venous return line. The tip of the venous cannula was cut to allow passage of the Intracath. When pulmonary artery pressure (PAP) was monitored, a Swan-Ganz catheter was introduced by the same means as the CVP line. Arterial pressure was monitored by a Sherwood arterial pressure monitoring catheter introduced through an arteriotomy in the left femoral artery and secured with a 3-0 silk tie. All pressure lines were connected to Statham P23dB transducers and recorded on a Hewlett-Packard Model 7700 recording system.
Extracorporeal Circuit
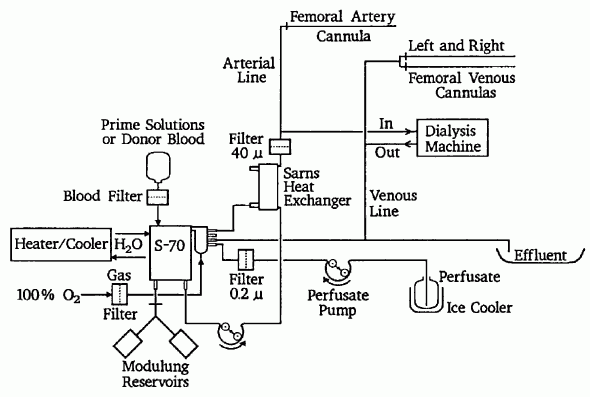
Figure 1: Diagram of the extracorporeal circuit.
The extracorporeal circuit for perfusion (Figure 1) contained a Shiley S-70 bubble oxygenator, Sarns stainless steel heat exchanger, Pall EC 1440 (40 micron) arterial line filter, and Travenol venous reservoir bags for storage of autologous blood. All tubing was Tygon S50-HL and connectors were from Cobe Laboratories. Arterial line blood/perfusate temperature was monitored using a Sci-Med adapter, Model TMA, and a Shiley TMI temperature monitor.
The circuit was primed with 1 liter of CPD-A preserved whole blood (converted prior to use with 5 ml of 10% calcium chloride and supplemented with 2,500 units of heparin) and 250 ml of 6% w/v hydroxyethyl starch (Mr 468 kDa; Hespan, McGaw Laboratories, Irvine, CA.) in normal saline with the addition of 23 mEq of sodium bicarbonate (total priming volume 1,275 ml). The prime was circulated and cooled to 15°C before initiation of partial bypass.
A Travenol RSP hemodialysis machine with an Erika HPF-200 dialyzer was connected via a standard hemodialysis loop to the arterial and venous lines of the extracorporeal circuit and was used during blood reperfusion to normalize electrolytes, pH, and hemocrit.
Cooling and Total Body Washout
Partial bypass using precooled perfusate was initiated when rectal temperatures were 28-32°C. Combined surface and perfusion cooling were continued until reaching rectal temperatures of 10-15°C, at which time circulatory arrest was instituted to allow exsanguination into the oxygenator reservoir. Blood was collected in Travenol reservoir bags and retained for reperfusion.
Total body washout (TBW) was achieved by perfusing 4 liters of precooled asanguineous perfusate in open circuit mode, collecting the venous blood for storage until rewarming and blood reperfusion. Perfusate was introduced into the oxygenator reservoir by roller pump through a Pall PP3802, 0.2 micron filter, to insure sterilization and particulate removal. When the venous return began to appear dilute, it was discarded. When the venous effluent appeared clear, the venous return line was redirected to the oxygenator for continued perfusion with recirculation. Asanguineous perfusion continued at 30 to 50 mm Hg arterial pressure, with flow rates of 1 to 1.5 l/min, down to a target temperature of 5°C. After keeping the dogs for the desired time at reduced temperatures, surface ice bags were removed and the Blanketrol blanket temperature was increased to start rewarming.
Blood reperfusion
When a rectal temperature of 10-12°C was achieved, the perfusion circuit was opened and the venous return was discarded until the perfusate level in the oxygenator was minimal. Autologous blood was then reintroduced into the oxygenator reservoir, and low flow perfusion continued until blood displaced perfusate in the venous return line. The venous return was then redirected to the oxygenator. Arterial blood flow was gradually increased to maintain mean arterial pressures between 60 and 80 mm Hg until partial bypass was discontinued.
During blood rewarming, hemodialysis was carried out as above using a bicarbonate-acetate solution (Erika EriLyte 8316 with K+ increased to 3.5 mM and Ca++ increased to 10.5 mM) to normalize serum electrolytes. Hematocrit was adjusted to 24-31% by ultrafiltration during dialysis.
When warming was complete, the animals were decannulated, and the femoral vessels were ligated. The muscle wound sites were closed with Vicryl and the skin was closed with 4-0 silk sutures. The suture line was sprayed with Aeroplast Dressing.
Laboratory tests
Blood/perfusate pH, pCO2 and pO2 measurements were made with a PHM72 digital analyzer and a BMS3 blood micro system (Radiometer) at a bath temperature of 37°C. Samples were drawn by syringe and analyzed immediately in the operating room. Hematocrits were run on a Select-A-Fuge Model 24 blood micro hematocrit centrifuge (Bio-Dynamics). Samples for hematological analysis were collected in Vacutainers and analyzed by Veterinary Research Laboratories (Anaheim, California).
Pathological follow-up
For light microscopic examination of tissue pathology, animals were anesthetized and perfused with 4% neutral formalin in 0.9% NaCl at 80-100 mmHg through a cannula placed in the ascending aorta. Tissues examined included the heart, lung, kidney, spleen, liver, pancreas, intestine, skeletal muscle, brain, spinal cord, and eyes.
Results
Eleven dogs were studied in all. The first was used in a pilot experiment involving only 1 hour of asanguineous perfusion. It recovered uneventfully and completely, but is excluded from further consideration as it did not meet our present protocol. Another dog was excluded because it died from an intestinal hemorrhage caused by a pre-existing coccidia infection that was discovered at necropsy. An additional three consecutive animals were considered technical exclusions as their deaths were caused by a ventilator malfunction that caused pneumothorax and pulmonary hemorrhage. All of the remaining 6 dogs survived without lasting neurological deficits, and the treatment and recovery of these animals are described here.
Temperature profiles during hypothermic low-flow perfusion are shown in Figure 2 and are summarized in Table 2 [PDF file]. For the group as a whole, the lowest mean esophageal temperature was 5.0 ± 0.9 C (± SD), and the duration of asanguineous perfusion was 4.3 ± 0.4 hours. Dog 5 was at or below 5°C (esophageal temperature) for the longest time, 152 minutes.
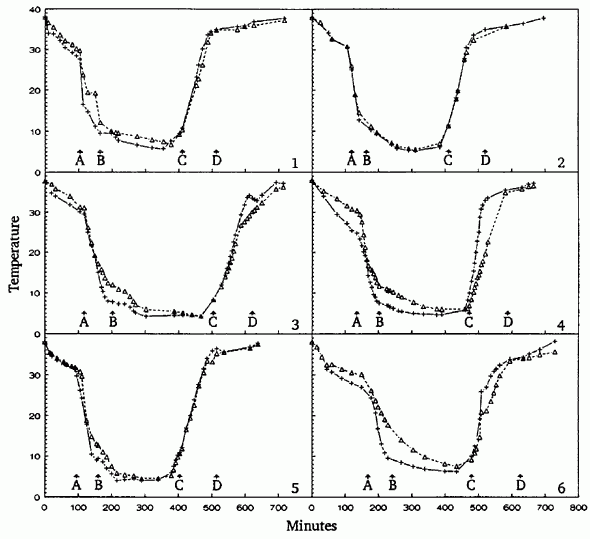
Figure 2: Temperature profiles for each of the six dogs subjected to hypothermia and total body washout. Surface cooling was begun at zero time; bypass was begun at A; TBW was begun at B; blood was reperfused at C; and the animals were taken off bypass at D. Plus sign indicates esophageal temperatures and delta sign indicates rectal temperatures.
Blood and perfusate samples were drawn before, during, and after TBW, and the results are shown in Figure 3 and Table 3 [PDF fle]. Hematocrits of 1.0 ± 0.7% were achieved. Lipase, SGOT, and SGPT were the enzymes most elevated after hypothermic exposure, but enzyme levels decreased to normal by day 12. In three animals, electrolytes were measured after blood reperfusion, pre- and post dialysis. Pre-dialysis serum potassium values in these three animals were 5.7, 11.4, and 7.2 mM. Approximately 30 minutes of hemodialysis during rewarming reduced serum potassium in these animals to 3.6, 4.8 and 5.2 mM respectively.
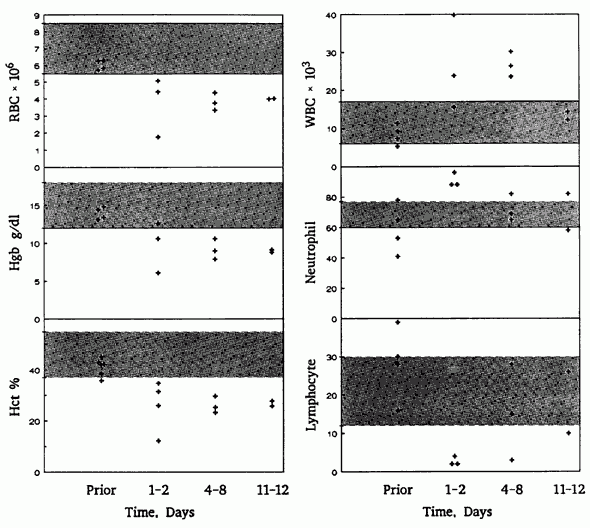
Figure 3: Hematological parameters measured prior to the experiment, 1 to 2 days following the experiment, at 4 to 8 days, and at 11 to 12 days. In each panel, the shaded area indicates normal range.
“Appropriate pH” was approximated during hypothermia: the temperature-corrected arterial pH of the first sample taken from each dog during cooling averaged 7.72, and the average pH at the lowest temperatures attained was 7.89, pH returning to a mean value of 7.44 at the end of the procedure.
Pulmonary edema has been a complicating factor in TBW in the past (13), but was not observed in the present study. Postoperative chest films of three of the dogs taken within 12 to 72 hours after wound closure showed all lung fields to be clear and normal. Further, appropriate blood gases were observed consistently upon weaning from cardiopulmonary bypass, and auscultation throughout the procedure gave negative results.
Oxygen delivery during TBW was calculated from pO2 measurements and oxygen solubility coefficients for plasma at each temperature (an approximation of oxygen solubility in the perfusate.) This estimated oxygen supply is compared in Figure 4 to the predicted temperature-specific whole-body and brain oxygen requirements. Based on this comparison, asanguineous perfusion consistently provided oxygen delivery above the calculated metabolic demand.
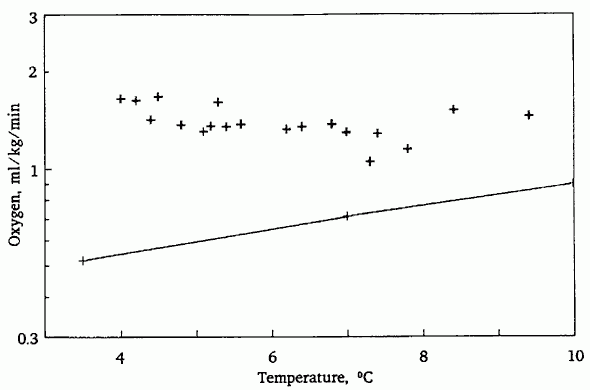
Figure 4: Oxygen requirement and supply during total body washout and hypothermia. The line shows the oxygen requirement at reduced temperatures calculated from the Q-10 rule. The points indicate the oxygen supply available from the perfusing solution during TBW, calculated from pO2 measurements made during perfusion.
Ventilatory compliance decreased markedly during bag-valve ventilation. As noted above, this was not due to pulmonary edema. Reduced compliance in deep hypothermia has been commonly observed and appears to be the result of generalized stiffening of the thoracic tissues. The solidification of subcutaneous fat was directly observed in the current study.
We noticed corneal flattening in these animals during profound hypothermia. This may have been the result of the high osmolality of our perfusate, which might be expected to cause ocular dehydration. As originally reported by Smith in a hamster model (22), lens opacity developed in our animals during deep hypothermia; this phenomenon appears to be caused by the reversible, thermally-driven precipitation of the gamma crystallins ( -III and -IV) (28) and is not considered an untoward sign. All opacities as well as ocular flattening resolved spontaneously upon warming and reintroduction of blood.
During blood reperfusion and rewarming, lash reflex, then corneal reflex, and finally spontaneous respiration returned. Heart beat with normal sinus rhythm resumed spontaneously in two dogs, and four dogs were defibrillated with external paddles when esophageal temperature reached 35°C and left ventricular fibrillation was identified by EKG.
Neurological recovery was generally satisfactory. None of our animals exhibited blindness or permanent neurological deficits. Three animals had names before the procedure, which they responded to after the procedure. Four animals were housebroken before hypothermia, and they remained housebroken afterwards. One animal had been trained to sit and heel on command and remembered this training after recovery. One dog also had excitement-induced (stress) incontinence prior to and following hypothermic TBW. More generally, the animals’ kennel behavior appeared to be normal after the procedure. Two dogs experienced post-operative seizures. The first was treated with Valium and pentobarbital, as needed, until the problem subsided on day 7. The second had two discrete seizures post-operatively without further incident and did not require treatment.
Two animals were ambulatory within a few hours of waking up, but the other four required intensive care for 24 hours after the procedure, and most dogs required several days to regain a normal gait. Most animals also required several weeks to overcome fatigue (diminished exercise tolerance and increased sleeping time after exercise).
Two dogs did not eat or drink normally in the immediate recovery period and were studied radiologically with barium contrast medium. These animals were found to have reduced intestinal motility (the transit time was 27 hours), but this resolved without treatment or complications, and normal food intake resumed. Two dogs retained urine and were catheterized for less than one day. Micturition was normal in the other four dogs.
Two animals developed infections at the groin wound sites. These infections were treated with cephalosporin antibiotics (Keflin and Mandol) and resolved. Normal hind-limb tenderness was observed secondary to bilateral ligation of the femoral vessels and resolved uneventfully.
One animal was sacrificed after six days to permit any short term effects of the procedure to be examined. Its liver was markedly depleted of glycogen (PAS stain), but all other tissues were histologically normal. Two of the remaining five animals were sacrificed at six months for histological examination. No changes were observed in the myocardium, lungs, liver, ileum, pancreas, spleen, kidneys, adrenals, or other abdominal and thoracic tissue. The eyes, optic nerves, cerebral cortex, hippocampus, cerebellum, brain stem, and spinal cord also appeared unremarkable. The remaining three animals were adopted as pets and were still alive and apparently healthy at the time this report was submitted (December, 1994).
Discussion
Profound hypothermia in dogs, without total body washout, was pioneered by Golan, et al., in 1955 (11) and continued by Kiyoshi, et al., in 1986 (16). However, clinical applications of hypothermia were restricted to temperatures well above the fibrillation threshold (23°C for humans and 19-26°C for dogs (24)) until the advent of cardiopulmonary bypass. Even current applications of hypothermia using cardiopulmonary bypass techniques seldom go below 15°C due to adverse hematological effects (15), and clinically acceptable hypothermic periods remain limited to less than 60 min. Profound hypothermia to temperatures as low as 5-7°C has been achievable only with total blood replacement, using delipidated plasma (12) or with synthetic solutions (9, 11, 14). Asanguineous perfusion (total body washout) using extracellular solutions began with the work of Neely and colleagues in 1968 (20) and was extended greatly by Klebanoff and his colleagues in the 1970s (12, 17, 18). Nevertheless, this technique until very recently has generally not eliminated lingering problems of elevated mortality and pulmonary, pancreatic, and cerebral edema as well as gastrointestinal hemorrhage (4, 12).
The intent of the experiments reported here was to test the hypothesis that prolonged ultraprofound hypothermia could be safely induced with the use of a simple “intracellular” perfusate broadly similar to clincally-used in vitro organ preservation solutions. This hypothesis is supported by the uniform survival of our animals after 5 hours of ultraprofound hypothermia near 5°C, a hypothermic “suspended animation” period 1.5 hours longer than (and a sustained degree of hypothermia significantly more profound than) has been previously described (26, 27). A number of factors may have contributed to the recovery of the dogs in this study.
The most fundamental explanation for recovery is presumably prevention of cell swelling by the use of an “intracellular” type perfusate with poorly permeating species. Until the work of Taylor et al. in 1994 (26, 27), safely sustainable hypothermic periods have been brief. The departure followed by Taylor’s group was the use of an “intracellular” type perfusate for such experiments. Control experiments involving use of an “extracellular” vs. “intracellular” perfusate in which other experimental conditions were unchanged strongly indicated that the nature of the perfusate used to sustain cellular viability and prevent cellular swelling is critical for a successful outcome (27). The perfusate employed by Taylor’s group is heavily based on the recent development of UW Solution (ViaspanTM, DuPont Medical Products, Wilmington, Delaware) with the omission of hydroxyethyl starch in favor of dextran 40. Largely because our experiments were carried out before the beneficial effects of the impermeants of UW Solution had been discovered, the primary impermeant species in SHP-1 was mannitol. This solute appeared to be sufficient to sustain the animals in this study and is noteworthy for its comparatively low cost and greater clinical familiarity.
Another important question is the role of the pH strategy used during deep hypothermia. We employed the alpha stat approach in which pH is allowed to rise to keep pace with the elevation in the pKa of water with increasing hypothermia, whereas other authors have used the poikilotherm strategy of maintaining absolute pH relatively constant so as to employ metabolic acidosis as an inhibitor of metabolism. While our experiemnts do not resolve the issue of which approach, if either, is superior, they do show that an alpha stat approach is compatible with a good outcome following ultraprofound hypothermia. The issue of proper pH strategy requires further attention.
In our experiments, hemodialysis was used to accomplish several important objectives that would have been much more awkward to achieve with other methods. In the experience of Taylor et al. (27), the 4 liters of Hypothermosol used at the lowest temperatures (7oC nadir) required a “chase” of 5 liters of a transitional low-potassium solution to remove the excess K+ contained in Hypothermosol, and in many instances this volume was insufficient to reduce potassium levels to below 10 meq/l. We found that dialysis could lower elevated potassium levels without the need for a transitional solution. In fact, because commercial dialysates contain very little potassium and calcium, we actually found it necessary to fortify the potassium and calcium concentrations in the commercial dialysate to avoid excessive depletion of these minerals. Dialysis was also helpful for following the alpha stat approach to pH control. In addition to directly adjusting pH with the bicarbonate of the dialysate, the use of acetate-rich dialysate provides a substrate for hepatic synthesis of additional bicarbonate. Further, dialysis removes lactic acid, which our subsequent experiments as well as the experiments of Klebanoff et al. have shown accumulates during hypothermic perfusion. Even with dialysis, control of pH required almost continuous addition of sodium hydroxide to the “recirculating” compartment of the dialysis machine to maintain pH at 7.4 at the end of warming as indicated by a pH probe in that compartment. Finally, we also used dialysis successfully to induce ultrafiltration to raise the hematocrit to more physiologic values during rewarming and to concentrate circulating oncotic agents.
While this study does not address the use of circulatory arrest following TBW, we consider this a fertile area for future research and see no reason why, in principle, application of techniques developed to facilitate extended hypothermic storage of solid organs for transplant can not be applied in a similar way to the whole organism. On the other hand, because synthetic perfusates are more expendable than blood, and are transparent, complete circulatory arrest is not necessarily required for deep hypothermic surgical repair procedures.
Acknowledgements
The authors wish to thank the following people for volunteering their time to assist in carrying out these experiments from July, 1984 to October, 1986: Scott Greene, Brenda Peters, Carlos Mondragon, Arthur McCombs, Sherry Cosgrove, Bill Jameson, Allen Lopp, Simon Carter, and Anna Schoppenhorst. We thank Clyde R. Goodheart, Gregory M. Fahy, and Paul Wakfer for assistance with the manuscript. Supported by grants from the ALE Foundation, Riverside, CA and the Life Extension Foundation, Hollywood, FL.
References
1. Agostini JC, Ramirez RG, Albert SN, Goldbaum LR, Absolon KB. Successful reversal of lethal carbon monoxide intoxication by total body asanguineous hypothermic perfusion. Surgery 1974;75:213-9.
2. Alpini G, Garrick RA, Jones MJ, et al. Water and nonelectrolyte permeability of isolated rat hepatocytes. Amer J Physiol 1986;251:872-82.
4. Bailes JE, Leavitt ML, Teeple E Jr, et al. Ultraprofound hypothermia with complete blood substitution in a canine model. J Neurosurg 1991;74:781-8.
5. Baumgartner WA, Silverberg GD, Ream AK, Jamieson SW, Tarabek J, Reitz BA. Reappraisal of cardiopulmonary bypass with deep hypothermia and circulatory arrest for complex neurosurgical operations. Surgery 1983;94:242-9.
6. Baumgartner WA, Williams GM, Fraser GD Jr, et al. Cardiopulmonary bypass with profound hypothermia. Transplantation 1989;47:123-7.
7. Barratt-Boyes BG, Neutze JM, Clarkson PM, et al. Repair of ventricular septal defect in the first two years of life using profound hypothermia-circulatory arrest techniques. Ann Surg 1976;184:376.
8. Belzer FO, Southard JH. Principles of solid organ preservation by cold storage. Transplantation 1988;45:673.
9. Connolly JE, Roy A, Guernsey JM, Stemmer EA. Bloodless surgery by means of profound hypothermia and circulatory arrest. Ann Surg 1965;162:724-36.
10. Ergin MA, O’Connor J, Guinto R, et al. Experience with profound hypothermia and circulatory arrest in the treatment of aneurysms of the aotic arch. J Thorac Cardiovasc Surg 1982;84:649-55.
11. Gollan F, Tysinger DS Jr, Grace JT, Kory RC, et al. Hypothermia of 1.5 C in dogs followed by survival. Amer J Physiol 1955;181:297-303.
12. Haff RC, Klebanoff G, Brown BG, Koreski WR. Asanguineous hypothermic perfusion as a means of total organism preservation. J Surg Res 1975;19:13-9.
13. Haneda K, Thomas R, Sands MP, Breaseale DG, et al. Whole body protection during three hours of total circulatory arrest: An experimental study. Cryobiol 1986;23:483-94.
14. Jesch F, Sunder-Plassmann L, Pohl U, Messmer K. Total body washout (TBW) and circulatory arrest in profound hypothermia. In: Messmer K, Schmid- Schebein H, eds. Intentional Hemodilution, Biblthca Haemat, Vol 41. Basel, Switzerland: 1975;209-24.
15. Keen G, Gerbode F. Observations on the microcirculation during profound hypothermia. J Thorac Cardiovasc Surg 1963;45:252-60.
16. Kiyoshi H, Thomas R, Sands MP, et al. Whole body protection during three hours of total circulatory arrest: An experimental study. Cryobiol 1986;23:483-94.
17. Klebanoff G. Infectious hepatitis complicated by coma: principles of management including the adjunctive use of asanguineous hypothermic total body perfusion. Resuscitation 1972;1:327-33.
18. Klebanoff G, Phillips J. Temporary suspension of animation using total body washout and hypothermia: A preliminary report. Cryobiology 1969;6:121-5.
19. Marshall FF, Reitz BA. Technique for removal of renal cell carcinoma with suprahepatic vena caval tumor thrombus. Urol Clin No Amer 1986;13:551-7.
20. Neely WA, Haining JL. Survival after suspension of perfusion during asanguineous cardiopulmonary bypass. Ann Thorac Surg 1968;5:222-7.
21. Sealy WC. Hypothermia: its possible role in cardiac surgery. Ann Thoracic Surg 1989;47:788-91.
22. Smith AU. Studies on golden hamsters during cooling to and rewarming from body temperatures below 0 C. II. Observations during and after resuscitation. Proc Roy Soc B 1956;145:407-426.
23. Smith AU. Viability of supercooled and frozen mammals. Ann NY Acad Sci 1959;80:291-300.
24. Southwick FS, Dalglish PH Jr. Recovery after prolonged asystolic cardiac arrest in profound hypothermia. JAMA 1980;243:1250-3.
25. Swain JA. Hypothermia and blood pH. Arch Intern Med 1988;148:1643-6.
26. Taylor, M.J., Bailes, J.E., Elrifai, A.M., et al. A new solution for life without blood: asanguineous low flow perfusion of a whole-body perfusate during 3 hours of cardiac arrest and profound hypothermia. Circulation (in press), 1994.
27. Taylor, M.J., Bailes, J.E., Elrifai, A.M., Shih, T.S., Teeple, E., Leavitt, M.L., Baust, J.G., and Maroon, J.C. Asanguineous whole body perfusion with a new intracellular acellular solution and ultraprofound hypothermia (7 C) provides cellular protection during 3.5 hours of cardiac arrest in a canine model. ASAIO J. (in press), 1994.
28. Wolanczyk JP, Abstender T, Bateman O, Duclos J. Further biophysical investigations into a family of eye-lens proteins: The -crystallins. Cryobiology 1991;28:560.
