Advances in Cryonics Protocols, 1990-2006
By Aschwin de Wolf & Chana Phaedra
Introduction
This paper presents a detailed review of the changes in stabilization, cryopreservation, and cryogenic cooldown protocols between 1990 and 2006. The cryopreservation of patient A-1049 in 1990 was described in the most comprehensive technical case report produced up to that time. This paper is intended to accompany the technical case report for the cryopreservation of patient A-1097 in 2006, which is the most comprehensive technical case report produced since 1990. Since both cases were neuropreservation cases, this paper emphasizes neuropreservation protocols.
General Protocol
The purpose of a human cryopreservation protocol is to preserve the brain in the best condition possible at cryogenic temperatures after medico-legal death is pronounced, in anticipation of subsequent future resuscitation. To this end, immediately after legal pronouncement of death, manual and mechanical cardiopulmonary support (CPS) is started to supply oxygen and nutrients to the cells, circulate stabilization medications, and to achieve circulation enhanced cooling of the patient to reduce metabolic rate. Upon arrival at the facility the patient’s head is selectively cooled to achieve rapid profound hypothermia prior to cephalic isolation. After cephalic isolation the patient’s head is washed out and perfused with a chilled vitrification agent to prevent ice formation during cooldown to cryogenic temperatures. The vitrification agent is introduced in a linear fashion to prevent dehydration induced osmotic shock. After terminal concentration of the vitrification agent has been reached, the patient is cooled down to cryogenic temperatures using convective cooling with liquid nitrogen vapor. Physiological data are collected throughout all procedures to monitor the condition of the patient and to assist personnel in real time interventions. Subsequently these data may help to evaluate both performance and protocol, and may facilitate future resuscitation.
Changes in Protocol
The most significant change in protocol was introduced in late 2000 when the organization switched from high molar glycerol cryopreservation to vitrification using cryoprotective agents designed to prevent the formation of ice crystals during cooldown to liquid nitrogen temperatures [1]. Initially this technology was only available to neuropreservation members and members who opted to use separate technologies for preserving the head and the rest of the body. In October 2005, Alcor announced perfusion of the head and body using a new vitrification agent, M22, that had been developed by the company 21st Century Medicine, Inc., for vitrification of transplantable organs in mainstream medicine. In published scientific literature, M22 allowed rabbit kidneys cooled to -45 degrees Celsius to be subsequently transplanted and function long-term as a sole kidney in recipient animals[2]. This was also achieved after cooling to -135 degrees Celsius (vitrification) in one reported instance[3].
Another major change in cryopreservation technology is the introduction of a subzero industrial chiller to assist in cooldown during cryoprotectant perfusion to reduce toxicity of the vitrification agent and minimize cold ischemic injury. Alcor also made a transition from the use of silicon oil cooling to nitrogen vapor cooling for neuro and whole body patients.
Improved Cryoprotective Agents
Up until 2000 Alcor patients were usually perfused with high concentrations of glycerol (approximately 7.0 molar). The resulting high toxicity, increased dehydration, and longer perfusion times (due to increased viscosity) were preferred to increased ice formation observed in experiments with lower glycerol concentrations [4].
Although the prospect of cooling a patient down to cryogenic temperatures without the formation of ice crystals has always been perceived as highly desirable, for many years this goal remained largely theoretical. Because water can only be vitrified employing extreme cooling rates, very high pressures, or using unworkable concentrations of glycerol, the task was to discover, or design, a solution that was able to vitrify in a realistic setting.
The first successful vitrification solution in cryobiology was VS1, designed by cryobiologist Greg Fahy while working at the American Red Cross. VS1 is a solution consisting of DMSO, acetamide, propylene glycol, and polyethylene glycol. VS1 was used to achieve reversible vitrification of mouse embryos in liquid nitrogen in 1985. The solution was modified for use in organ vitrification by replacing the acetamide with formamide, and increasing the overall concentration of solutes to allow cooling and rewarming at slower rates. The resulting solutions, VS4 and VS41A, were still unsuitable for cryonics use because of cooling rate requirements.
With Fahy’s move to 21st Century Medicine in the late 1990s, the science of organ vitrification entered a new area of unprecedented productivity and fundamental discoveries. Systematic study of the physical and chemical properties of vitrification solutions led to the rational design of a series of improved vitrification agents.
A major step forward in reducing non-specific cryoprotectant toxicity was made in predicting the toxicity of cryoprotectant mixtures using a compositional variable called qv*, where q can be derived by dividing the molarity of water (Mw) by the molarity of all polar groups on the permeating cryoprotectants (Mpg) in the vitrification solution, where v stands for the concentration needed to vitrify, and the asterisk means that the concentration needed to vitrify is arrived at utilizing a standard slow to moderate cooling rate. Using qv*, 21st Century Medicine researchers found that solutions with a high qv* are more toxic than solutions a low qv*, or as the variable implies, that weak glass formers produce less toxicity.
A proposed explanation for this causal relationship is that vitrification solutions containing permeating cryoprotectants with a higher qv* leave less water available for hydrating biomolecules, compromising intracellular viability. It is important to note that qv* is not useful for predicting specific cryoprotectant toxicity associated with other mechanisms of toxicity [5].
These concepts were vindicated by the success in formulating superior vitrification solutions with lower toxicity, such as VEG, in which the weak glass former, ethylene glycol, was substituted for the strong glass former, propylene glycol. Although more concentrated than VS4A1, derivatives of VEG resulted in higher viability than the former, as measured by K+/Na+ ratios.
Without the presence of ice nucleators (e.g., impurities, surfaces), pure water can be supercooled to -42 degrees Celsius. This temperature can be lowered further by adding cryoprotectants like glycerol or DMSO. In biological materials (and vitrification solutions) the concept of homogeneous nucleation is of limited use, and nucleator-induced heterogeneous cooling at much higher temperatures should be expected. Therefore, inhibiting heterogeneous nucleation can contribute to better vitrification solutions by lowering the minimum cooling and warming rates.
Naturally occurring anti-freeze proteins that inhibit heterogeneous nucleation have been suggested to assist in vitrification of complex biological systems. But limited supply and the costs of such anti-freeze proteins have been major obstacles in using them for organ preservation. In 2000, Brian Wowk et al., proposed that the property of selective binding to heterogeneous nucleators could also be achieved by using synthetic polymers. It was found that a copolymer consisting of 80% w/w low molecular weight polyvinyl alcohol (PVA) and 20% vinyl acetate substantially reduced ice formation when added to standard cryoprotectants. This copolymer is now being sold as Supercool X-1000 by 21st Century Medicine.
Another polymer, polyglycerol (PGL), was found to selectively inhibit bacterial ice nucleation and complement the more general action of PVA in inhibiting ice nucleation. This polymer is currently being sold as Supercool Z-1000, and the combination of the two produces superior inhibition of ice formation than either of the two polymers alone. By lowering the minimum concentration of cryoprotectant(s) needed to vitrify, and thus lowering the total viscosity of the solution, the addition of X-1000 and Z-1000 represented another elegant step towards reversible organ vitrification [6].
Concentrated aqueous solutions of X-1000 tend to become turbid after preparation. In 2005, Wowk isolated the turbidity-causing condensed particles from a 20% w/w solution of X-1000 and discovered that these particles, although less water soluble and more self-associating, contributed disproportionately to the ice blocking properties of X-1000. The mechanisms and practical applications of this finding are currently being explored [7].
The first vitrification solution to be introduced to cryonics was B2C, a highly concentrated “hyperstable” variant of VM3, which is a more stable and enhanced version of VEG that includes the polymer polyvinylpyrrolidone K12 (PVP K12), and the two ice blockers, X-1000 and Z-1000 as additional components. The objective of Alcor’s first vitrification agent was to eliminate ice formation and achieve good structural preservation of the brain. Preserving viability by contemporary criteria was not assumed to be possible with B2C. Another limitation of B2C was that it produced edema in whole body patients and thus was not available to whole body patients.
In late 2005, Alcor introduced M22, a vitrification agent that reflects recent research at 21st Century Medicine. M22 offers the following advantages over B2C [8, 9]:
- Solution of published composition.
- Published success recovering kidneys from -45°C and -135°C.
- Published success of structural brain vitrification.
- Low toxicity per published studies.
- Low viscosity, resulting in faster perfusions.
- Compatible with additives permitting whole body perfusion.
M22 consists of the non-penetrating solutes polyvinyl pyrrolidone K12, X-1000 and Z-1000, and the penetrating solutes dimethyl sulfoxide (DMSO), formamide, ethylene glycol, N-methylformamide and the glycerol derivative 1,3-dimethoxy-2-propanol.
Table 1. The published formula of M22
| Dimethyl sulfoxide | 22.305% w/v |
| Formamide | 12.858% |
| Ethylene glycol | 16.837% |
| N-methylformamide | 3% |
| 3-methoxy-1,2-propanediol | 4% |
| Polyvinyl pyrrolidone K12 | 2.8% |
| X-1000 ice blocker | 1% |
| Z-1000 ice blocker | 2% |
Table 2. The formula of B1
| Chemical | MW | Molar Conc. | Grams/Liter |
| Glucose | 180.16 | 90 mM | 16.214 |
| Mannitol | 182.17 | 45 mM | 8.198 |
| Alpha-Lactose Monohydrate | 360.31 | 45 mM | 16.214 |
| Potassium Chloride | 74.55 | 28.2 mM | 2.102 |
| Potassium phosphate dibasic trihydrate | 228.22 | 7.2 mM | 1.643 |
| Gluthathione reduced) | 307.32 | 5 mM | 1.537 |
| Adenine HCl | 171.59 | 1 mM | 0.172 |
| Sodium Bicarbonate | 84.01 | 10 mM | 0.840 |
| Calcium Chloride Dihydrate | 0.147 | ||
| 10% w/v | 147.01 | 1.0 mM | 1.47 ml |
| Magnesium Chloride Hexahydrate | 0.407 | ||
| 20% w/v | 203.3 | 2.0 mM | 2.035 ml |
| Proprietary Additive |
The current protocol for perfusing the patient with M22 is to wash out the blood with B1 and start perfusion with 100% B1 around +3.5 degrees Celsius. Over a period of about 90 minutes a concentrated form of M22 (125%) is gradually added to approximate a linear increase to allow the cells to equilibrate and avoid osmotic injury. When 50% of target concentration is reached, the increase is paused to allow time for the venous effluent concentration to approach the arterial concentration and lower the perfusion temperature to -3 Celsius. When the venous effluent concentration has approached the arterial concentration, the concentration is rapidly increased to 100% target concentration to minimize the toxic effects of the vitrification agent at higher concentrations. At this point the arterial concentration is held between 100% and 105% as long needed, but not exceeding 5 hours, for the venous effluent to reach 100% target concentration.
The prior state of the art in neuropreservation was to place an arterial cannula in the aorta and a venous cannula in the superior vena cava. Systemic and upper body perfusion was prevented by ligating the descending aorta and the peripheral vessels. The current technique for neuropreservation is to separate the head from the rest of the body prior to cryoprotectant perfusion. The head is secured in a cephalic enclosure and all four vessels are cannulated. Venous return can be achieved through both jugular veins or can be drained into a tray and returned to the recirculating reservoir.
Figure 1. The cephalic enclosure used for neuropreservation

The circuit that is used for perfusion of the vitrification agent basically reflects the same parameters as previous circuits. A roller pump withdraws a concentrated form of the cryoprotectant agent (CPA) from a reservoir and feeds this into the recirculating reservoir where the CPA is instantaneously mixed with the carrier solution. A second pump is used to force the fluid through a 40 micron filter and heat exchanger into the patient. But unlike the circuit for whole body patients, venous return does not exit the patient through venous cannulae but is drained onto a tray. Most of the volume is returned to the recirculating reservoir and some of it is discarded. The circuit monitors pressure and temperature and can be used to take manual samples to determine the refractive index or other measurements.
Cool down of the perfusate below zero degrees Celsius is achieved by using a sub-zero industrial chiller. Use of the chiller in conjunction with cryoprotection is similar to the use of ice water to cool the heat exchanger in an extracorporeal perfusion circuit. The chiller uses a standard water-based liquid coolant like ethylene glycol that runs through the heat exchanger in the vitrification circuit and returns to the chiller again.
Figure 2. The chiller used for subzero cool down of the vitrification agent.

Cooldown to cryogenic temperatures in neuropreservation patients is achieved by moving the cephalon to an LR-40 dewar with a modified lid. This lid uses a computer controlled valve to inject liquid nitrogen into the dewar. Because the temperature difference between the interior of the dewar and the liquid nitrogen, the nitrogen vaporizes and draws heat from the patient. A fan on the lid circulates the vapor to enhance cooling. Because vitrification requires rapid cooling, the temperature is dropped rapidly until around -110 degrees Celsius, after which the temperature is dropped more slowly to reduce thermal stress and fracturing. This cooling technology is not sufficient to cool down the core temperature of the patient completely to liquid nitrogen temperature. The final descent from around -190 degrees Celsius to -196 degrees Celsius is achieved by gradually filling the dewar with liquid nitrogen.
Figure 3. The modified LR-40 dewar connected to a liquid nitrogen tank.

Figure 4. The modified lid to cool down the patient.

Concurrent with the introduction of M22, a new patient enclosure and cool down box were introduced to keep the patient cold during cryoprotective perfusion and to match the lower subzero temperatures that are used during the final stage of cryoprotectant perfusion. A more detailed description of these new technologies will be found in future whole body case reports.
Changes in stabilization and transport protocol
Changes in stabilization and transport technology have been relatively minor compared to the changes in cryopreservation and cooling technology.
In early 2003, Alcor acquired a new mechanical cardiopulmonary resuscitation unit from Sweden called the LUCAS. Like the modified Michigan Instruments “Thumper” that is used in cryonics, the LUCAS delivers active compression-decompression cardiopulmonary support by pneumatically compressing and decompressing the chest between a suction cup and the backboard at a consistent rate of 100 compressions per minute and a compression depth of about 4-5 cm (depending on patient body weight). Some clear advantages of the LUCAS include price, size (<445 mm), and weight (6.5 kg). Some limitations include the lack of an integrated ventilation option, necessitating a separate ventilator, and a sternum height range of 17-27 cm, preventing its use on obese patients. The LUCAS is currently the default CPS device in the Alcor rescue vehicle.
Figure 5: The LUCAS mechanical chest compressor.

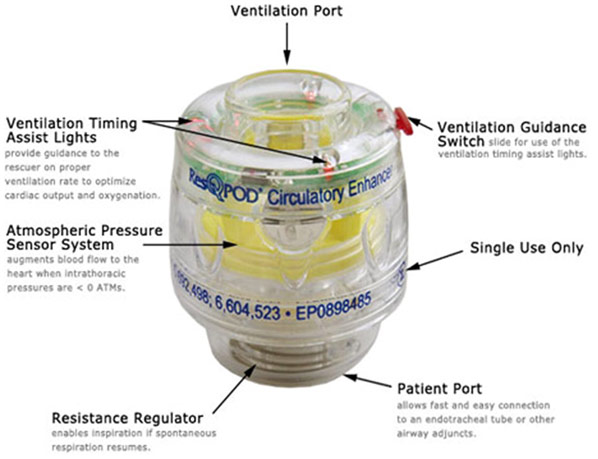
A new airway adjunct designed to optimize cardiac preload is the inspiratory impedance threshold valve. The valve is placed between the airway of the patient and the ventilation source and prevents air entering the patient during the recoil phase of chest compressions. As a result, intrathoracic pressure is reduced, improving venous return to the heart. In the late nineties, Michael Darwin recognized the potential value of this mechanism, and built the first prototype impedance valve for use in human cryopreservation. In 2005, Alcor added the first commercially available impedance valve, the ResQPOD Circulatory Enhancer, to its stabilization protocol. Positive findings using this airway adjunct, in conventional CPR or in conjunction with ACD-CPR, culminated in a recommendation of the impedance valve in the American Heart Association’s 2005 guidelines for cardiopulmonary resuscitation.
Figure 6: The ResQPOD circulatory enhancer.
Reflecting the need for improved data acquisition, Alcor has added the CO2SMO PLUS! to its stabilization monitoring equipment. The CO2SMO does capnography, pulse oximetry, and gives a comprehensive non-invasive, continuous respiratory profile. The CO2SMO operates by connecting a respiratory sensor to the patient’s ventilation circuit and connecting the pulse oximeter sensor to a finger or earlobe.
Figure 7: The CO2SMO PLUS!

Changes in medication protocol
Human cryopreservation medications protocol has typically consisted of a core group of medications to reduce cerebral metabolic demand, prevent and reverse blood clotting, restore blood volume, support circulation, stabilize pH, and a combination of neuroprotective agents to mitigate cerebral ischemia. Alcor’s cryopreservation stabilization medication protocol has been revised extensively since the last technical case report. The new protocol was developed in consultation with Critical Care Research, Inc., a company specializing in cerebral ischemia and resuscitation research.
The most important additions include substitution of the non-controlled general anesthetic, propofol, for potassium chloride and sodium pentobarbital, addition of the anti-platelet agent aspirin, the vasopressor vasopressin, the superoxide dismutase mimetic 4-Hydroxy Tempo (TEMPOL), the antioxidant cocktail VitalOxy, the iNos inhibitor SMT, the excitotoxity inhibitor kynurenine, the PARP inhibitor niacinamide and the routine use of the potent anti-coagulant citrate-dextrose.
Propofol is a rapidly acting lipid soluble intravenous anaesthetic that enhances the inhibitory synapses in the brain. Propofol is given for two reasons. The first reason is to reduce metabolism in the brain. The second reason is to prevent the theoretical possibility of any recovery of awareness during aggressive cardiopulmonary support, however unlikely it may be. Propofol also has antioxidant and free radical scavenging properties. There is also evidence that propofol delays the onset of excitotoxic neuronal death and reduces peroxynitrite-mediated apoptosis. The major disadvantage of propofol, however, is that it produces a decrease in arterial pressure and peripheral resistance.
Aspirin is an antiplatelet agent that irreversibly acetylates platelet adhesion factors.
Vasopressin is a vasopressor that is used to enhance cardiopulmonary support by increasing myocardial and cerebral perfusion. Because vasopressin targets the non-adrenergic V1 receptors, it is also effective in ischemia-induced acidosis. Another advantage of vasopressin is that it has a longer half-life than epinephrine and reduces the need for short-interval intermittent administration to support blood pressure.
S-methylthiourea (SMT), an inducible nitric oxide synthase inhibitor, is primarily used to mitigate inducible nitric oxide production and associated formation of the peroxynitrite radical. SMT also increases mean arterial pressure.
Kynurenine increases production of kynurenic acid, an endogenous antagonist of excitatory amino acid induced excitotoxicity, one of the upstream events in cerebral ischemia.
4-Hydroxy-Tempo (TEMPOL) is a low molecular weight superoxide scavenger. Ischemia-reperfusion-induced free radical generation is further mitigated by a proprietary antioxidant cocktail called Vital-Oxy. Vital-Oxy contains popular natural antioxidants like D-alpha tocopherol (Vitamin E), melatonin and the free radical spin trapping agent alpha Phenyl t-Butyl Nitrone (PBN). Vital-Oxy also includes the anti-inflammatory drug carprofen.
Another recent addition to this multi-modal treatment of cerebral ischemia is the PARP-inhibitor Niacinamide (vitamin B3). The hyperactivation of the DNA repair enzyme poly (ADP-ribose) polymerase (PARP) during ischemia leads to a rapid depletion of the major energy sources of the cell. Studies of PARP-inhibitors in animal models and “knock-out” mice (mice with inactivated PARP genes) indicate the potential of PARP inhibition in mitigating cerebral ischemia. One advantage of PARP inhibitors is that PARP activation is a final common pathway in many of the events of the ischemic cascade, potentially offering a greater degree of protection and providing a longer window of opportunity in mitigating cerebral ischemia.
Citrate-dextrose is a potent anti-coagulant that is used to dissolve the NiKy (Niacinimade and Kynurenine) combo medication, prevent blood coagulation, and mitigate calcium induced ischemic / reperfusion injury.
Categories of medications that are no longer being administered include neuromuscular blocking/anti-shivering agents, calcium channel blockers, iron chelators and cell membrane stabilizers.
Table 3: Alcor’s complete stabilization medications list
Propofol
Streptokinase
Heparin
Vital-Oxy (Vitamin E, Melatonin, PBN and Carprofen)
Epinephrine
Vasopressin
SMT (S-methylthiourea)
NiKy (Niacinimide & l-Kynurenine)
Citrate-Dextrose (solvent for NiKy)
4-Hydroxy-TEMPO (Tempol)
Gentamicin
THAM PLUS (Tromethamine plus Aspirin)
Hetastarch
Mannitol
Maalox
Gaining access to the circulatory system of a patient to deliver these medications and fluids has often been a challenge during Alcor cases. Many patients have advanced arteriosclerosis and are severely dehydrated at the time of pronouncement, presenting a serious and time-consuming obstacle for achieving intravenous access by even the most skilled team members. Unless medical staff can be persuaded to leave an IV line in place prior to legal death, attempts to place an IV have often interfered with the goal of rapid stabilization. Reflecting a renewed interest in emergency medicine to administer medications and fluids through the bone marrow, Alcor has recently adopted a technology to access the circulatory system through the sternum called the F.A.S.T.1 (First Access for Shock and Trauma). Sternal intraosseous infusion is expected to reduce the time to establish vascular access, in addition to other advantages such as the ability to infuse larger volumes.
This intraosseous infusion device is relatively easy to place. After prepping the site of insertion, a multi-needle device is used to place a tube in the sternal bone marrow through the manubrium, the top bone of the sternum. After placing a dome over the site of access to protect the tube from becoming dislodged, the tube can be connected to a regular IV line to start infusions. Flows of 250/ml per minute have been delivered through the F.A.S.T.1.
The following images illustrate how this device is used.
Figure 8: The F.A.S.T.1.
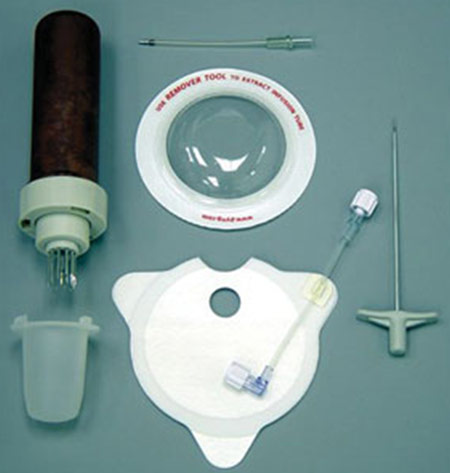
Figure 9: Diagram showing how to use the F.A.S.T.1.
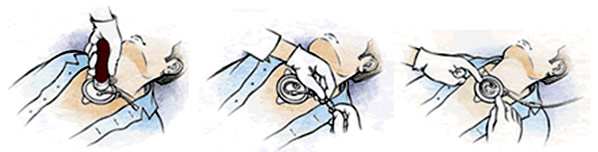
Figure 10: Illustration of intraosseous (IO) fluid administration using the F.A.S.T.1.

Alcor also added a portable bedside blood gas analyzer, the i-STAT, to its stabilization equipment. Fort the first time in cryonics, real-time blood gas and electrolytes measurements during stabilization and transport will be possible. Extensive discussion of the technology and measurements obtained will be reported in future case reports.
- Chamberlain, Fred. “Vitrification arrives: new technology preserves patients without ice damage.” Cryonics, 4th qtr, 2000, 21: 4, pp. 4-9.
- Fahy GM, Wowk B, Wu J, Phan J, Rasch C, Chang A, Zendejas E. Cryopreservation of organs by vitrification: perspectives and recent advances. Cryobiology, 2004 Apr;48(2):157-78.
- Fahy GM, Wowk B, Pagotan R, Chang A, Phan J, Thomson B, Phan L. Physical and biological aspects of renal vitrification. Organogenesis. 2009 Jul-Sep;5(3):167-75.
- Fahy, G.M. “A personal view of the Alcor research fund-raiser.” Cryonics, Volume 12, December 1991, Issue 137, pp. 13-14.
- Fahy GM, Wowk B, Wu J, Paynter S. Improved vitrification solutions based on the predictability of vitrification solution toxicity. Cryobiology, 2004 Feb;48(1):22-35.
- Wowk B, Leitl E, Rasch CM, Mesbah-Karimi N, Harris SB, Fahy GM. Vitrification enhancement by synthetic ice blocking agents. Cryobiology. 2000 May;40(3):228-36.
- Wowk B. Anomalous high activity of a subfraction of polyvinyl alcohol ice blocker. Cryobiology. 2005 Jun;50(3):325-31.
- Gomez-Angelats M, Cidlowski JA. Cell volume control and signal transduction in apoptosis. Toxicologic Pathology. 2002 Sep-Oct;30(5):541-51.
- Schliess F, Haussinger D. The cellular hydration state: a critical determinant for cell death and survival. Biological Chemistry. 2002 Mar-Apr;383(3-4):577-83.
